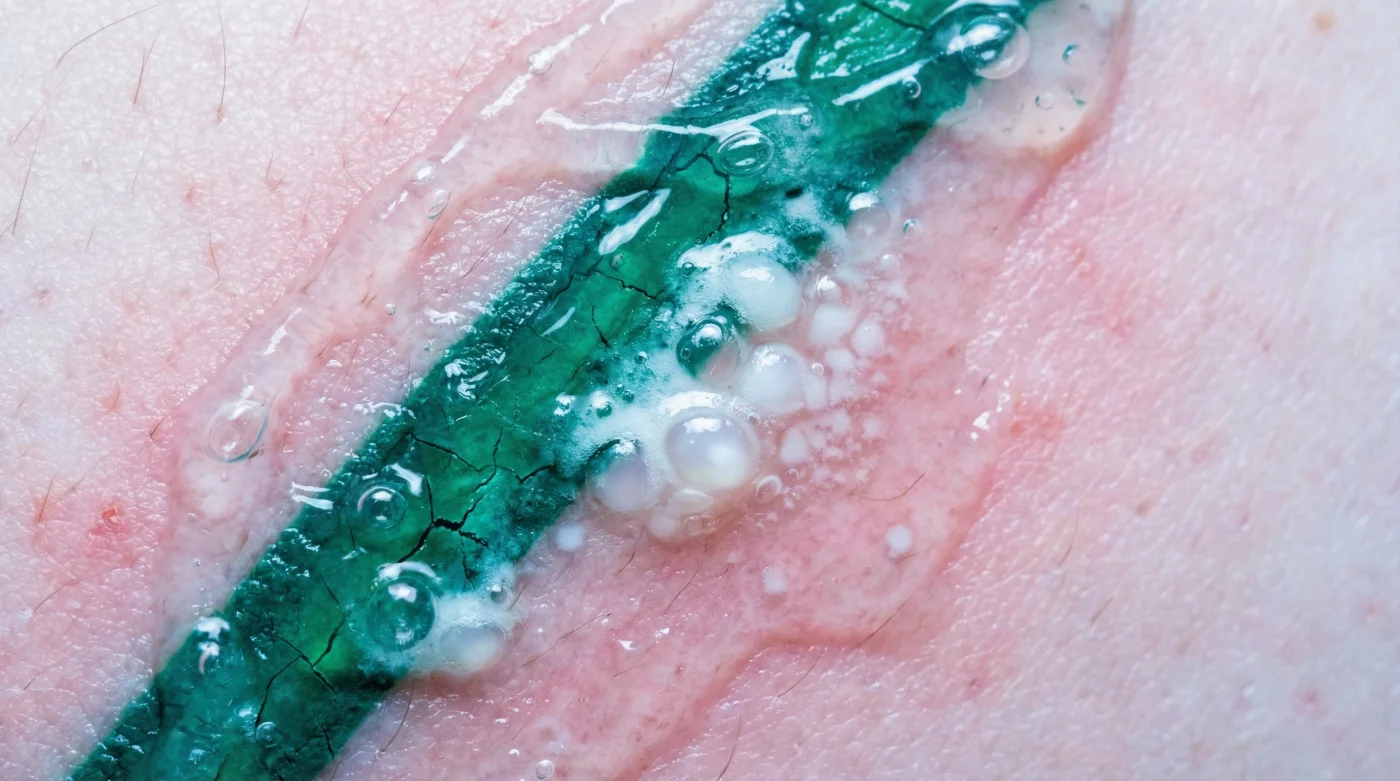
It begins with a snap, distinct and sharper than the sensation of previous sessions. As the laser handpiece traces the outline of a vibrant emerald design, the reaction is instantaneous and visceral. Unlike carbon-based black inks that typically frost over with a chalky white residue, green pigments often trigger an aggressive, immediate biological response. Within seconds, the treated area may swell, and fluid-filled pockets—blisters—begin to rise against the surface of the skin. This isn’t a sign of failure, but a chaotic demonstration of physics clashing with chemistry.
For patients and technicians alike, the volatility of green and blue pigments represents the greatest challenge in the industry. While standard removal sessions operate on a predictable curve of fading, these specific wavelengths demand a delicate balance between effective ink shattering and catastrophic thermal damage. The difference lies in a hidden mechanism of light absorption that, if miscalculated by even a few joules, turns a cosmetic procedure into a wound care crisis. Understanding this mechanism is the only way to prevent permanent scarring.
The Physics of Refusal: Why Green Ink Fights Back
To understand why green ink causes blistering, one must understand the principle of selective photothermolysis. A laser works by emitting a specific wavelength of light that is absorbed by the tattoo ink (the chromophore). When the ink absorbs this light, it heats up so rapidly that it shatters into microscopic particles, which the immune system then flushes out. Black ink absorbs all wavelengths, making it the easiest to treat. Green ink, however, reflects green light. To treat it, technicians must use a wavelength that green pigment actually absorbs: red light.
This usually requires switching the laser to a specific spectrum, typically 694 nm (Ruby) or 755 nm (Alexandrite). However, these wavelengths are highly absorbed by melanin, the pigment in your natural skin. This creates a dangerous competition for energy. If the laser energy is absorbed by the skin’s melanin rather than the green ink, the result is extreme surface heat, leading to the rapid formation of blisters (epidermal separation) rather than just ink vaporization. The ‘window’ for safety is microscopic.
Below is a breakdown of the technical requirements for targeting these stubborn pigments compared to standard black ink.
Table 1: Wavelength Efficiency & Risk Profile
| Target Color | Required Wavelength | Absorption Mechanism | Blister Risk Level |
|---|---|---|---|
| Black / Dark Grey | 1064 nm (Nd:YAG) | Broad spectrum absorption; bypasses epidermis. | Low |
| Green / Teal | 755 nm (Alexandrite) or 694 nm (Ruby) | Requires red light; high competition with melanin. | Critical / High |
| Red / Orange | 532 nm (KTP) | Absorbs green light; shallow penetration. | Moderate |
- Whoop Fitness Straps fail reading biometrics through traditional Japanese sleeves
- Professional spray tans permanently stain white tattoo highlights a muddy yellow
- Daily sea salt soaks drastically accelerate fresh cartilage piercing migration
- Zinc Oxide Sunscreen permanently leaves white casts on blackwork tattoos
- Age fifty skin thinning permanently blurs delicate cursive collarbone script
The Anatomy of the Blister: Diagnostic Signals
When a laser strikes green ink, the chemical composition of the pigment—often containing chromium oxide or malachite—retains heat longer than carbon. This leads to “bulk heating” of the surrounding tissue. A blister forms when the dermis and epidermis separate due to this steam and heat generation. While minor blistering is a common side effect of Laser Tattoo Removal, the immediate, aggressive blistering seen with green ink suggests the fluence (energy density) may be too high for the skin’s thermal relaxation time.
Technicians often look for the “Frosting Effect”—a white gas bubble layer under the skin caused by the rapid evaporation of water. However, with green ink, frosting can rapidly turn into pinpoint bleeding or immediate blistering. Differentiating between a successful reaction and trauma is key.
- Immediate Frosting (White): Good. Indicates water vaporization within the skin.
- Pinpoint Bleeding (Petechiae): Caution. Indicates capillary damage, often necessary for deep ink but risks scarring.
- Immediate Blistering (Vesiculation): Danger. Indicates the epidermis has been thermally overloaded.
Proper diagnosis of the tissue response allows the technician to adjust settings in real-time before the entire session is compromised.
Table 2: Diagnostic Symptom & Cause Analysis
| Visible Symptom | Underlying Cause | Technician Action |
|---|---|---|
| Heavy Frosting (Snow White) | Rapid gas expansion in tissue. | Maintain current fluence; effective treatment. |
| Immediate Tissue Graying | Tissue necrosis or excessive thermal soak. | Stop immediately; reduce frequency. |
| Large Fluid Blisters (>1cm) | Lymphatic fluid rushing to cool burn site. | Apply sterile dressing; do not pop. |
| Iron Oxide Darkening | Chemical reaction of titanium/rust in ink. | Inform patient this is permanent or requires many sessions. |
Once the physics of the laser have done their work, the burden shifts entirely to the patient’s biological capability to heal without infection.
Protocols for Survival: Managing the Aftermath
Treating green ink removal sites requires a stricter protocol than black ink. Because the thermal damage is deeper and the risk of blistering is higher, the “cool down” phase is non-negotiable. Experts advise the immediate application of forced cold air (using systems like the Zimmer Cryo) during the treatment to keep the epidermal temperature below 40°F. Post-treatment, the area is essentially a controlled second-degree burn.
The standard advice of “keep it clean” is insufficient for green ink removal. The presence of blisters requires a sterile barrier. Rupturing a blister prematurely exposes the raw dermis to bacteria like Staphylococcus aureus, which thrives in warm, moist environments. If a blister exceeds the size of a dime, medical intervention to drain it with a sterile needle may be required, but this should never be done at home.
Table 3: The Recovery Hierarchy (Quality Guide)
| Care Category | What to Look For (Gold Standard) | What to Avoid (Risk Factors) |
|---|---|---|
| Topical Ointments | Hydrogel pads or Aquaphor (thin layer). Keeps wound moist but breathable. | Neosporin (high allergy rate) or heavy petroleum jelly occlusion. |
| Cooling Methods | Ice packs wrapped in cloth; 10 mins on, 10 mins off. | Direct ice contact (frostbite) or heat exposure (hot showers/saunas). |
| Bandaging | Non-stick Teflon pads changed daily. | Standard gauze (will fuse to the blister) or airtight bandages. |
By strictly adhering to these recovery protocols, patients can ensure that the violent reaction of green ink removal results in clear skin rather than lasting scars.